
Menstrual health is an essential aspect of women's health that often goes underappreciated. For immigrant and refugee women in particular, managing menstrual health presents unique challenges. Cultural differences, language barriers and limited resources all contribute to these challenges.
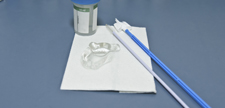
In the landscape of women's health, the Pap smear stands as a robust diagnostic tool, particularly vital in the prevention of cervical cancer. This article explores the complexities of Pap smears, highlighting their pivotal role in early detection and underscoring the nuanced influence of public policies in broadening accessibility to these screenings.

During my Women’s Health Education Program (WHEP) elective, I had the privilege of spending a month learning from international board-certified lactation consultants and caring for lactating parents at St. Christopher’s Hospital for Children. As a medical student, I knew only that chest feeding led to better health outcomes. However, what I now know is that U.S. parents who chest feed tend to be of higher socioeconomic statuses, be disproportionately white, and have job flexibility, social support, low stress levels and higher levels of education.

In the scope of women’s reproductive rights in the United States, a topic that is often overlooked is the country’s history of sterilization abuse. Minoritized women in the U.S. have historically been more likely to be sterilized than other women, often without their knowledge or consent. One aspect of the women’s health movement in the 1970s was to address these injustices, and this fight was led by Helen Rodríguez Trías, MD.

HIV is criminalized when people who are HIV positive can face criminal charges for engaging in acts not considered criminal if done by a person who is HIV negative.

For far too long disparities in the health care system, whether it was race, socioeconomic class or gender identity, have had a major impact on patients. Today we still see disproportionate measures when it comes to cancer and how it is diagnosed and treated. Breast cancer is the most common non-cutaneous cancer, with hundreds of thousands of new cases each year. Due to the increase in early detection and more effective treatments, the overall mortality rate due to breast cancer has decreased over the years.

Rising temperatures, sinking cities and increased natural disasters show the necessity of addressing climate change today. While these issues have sparked a global uproar and propelled action among world leaders, an insidious component of climate change lurks beneath the surface of melting ice and raging fires. Climate change highlights inequality and demonstrates the vulnerability of certain regions and populations.

Husband. Visionary. Social entrepreneur. One of 2014 Time Magazine’s 100 Most Influential People in the World. Recipient of the Padma Shri (the fourth highest civilian award) from the government of India in 2016. Subject of the 2018 short film “Period. End of Sentence.” as well as the critically and commercially successful 2018 Bollywood film “Pad Man” starring Bollywood star Akshay Kumar.

Period poverty is the lack of accessibility or affordability of menstrual hygiene tools and educational material, such as sanitary products, washing facilities and waste management.

The health benefits of breastfeeding for both mother and infant have been well-touted for years. Based on these undeniable benefits, the American Academy of Pediatrics recommends exclusive breastfeeding for the first six months of life and continuation of breastfeeding until two years of age or beyond, a recent revision from the previous recommendation of continued breastfeeding for the first year of life or longer.

Amidst anti-transgender legislation and don’t-say-gay bans, it is vital to consider the social and public health implications of attempts to minimize or even eliminate the experience of gender and sexual minorities. Transgender, or trans, individuals are those whose gender expression or identity differs from what they were assigned at birth.

“Breast is best” is a common phrase used to promote breastfeeding. However, providers should still be cognizant of the barriers to breastfeeding and the shame that mothers may feel when they are unable to or prefer not to breastfeed.