
In a world where systemic barriers in health care persist and public trust continues to fray, few voices cut through the noise with the clarity and conviction of Dr. Ala Stanford. At this year’s United Nation World Immunization Shot@Life event at Drexel on April 30, 2025, students and attendees had the profound privilege of hearing from the renowned pediatric surgeon, advocate and national leader in health equity during her keynote address — a talk that was as deeply personal as it was professionally inspiring.

Unfortunately, it’s not just the availability of abortion care that will impact the lives of birthing people in these states. After Dobbs, states with abortion bans in place experienced a decrease in the number of MD applicants for residency programs located in those states, particularly OB/GYN programs.
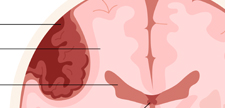
The Depo-Provera shot is a very common form of birth control that contains the progestin medroxyprogesterone acetate. This hormone mimics progesterone, binding to the progesterone receptor and essentially functioning the same way as the hormone. As a form of birth control, there are several functions of this injection. It works to prevent ovulation, preventing the release of an egg from the ovary.
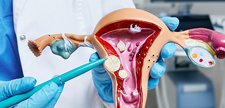
Uterine fibroids, also known as leiomyomas, are the most common benign (noncancerous) tumors made of smooth muscle and connective tissue that develop in the myometrium layer of the uterus. They are the most common pelvic tumors among women of reproductive age, affecting more than 70% of women worldwide.

HIV is criminalized when people who are HIV positive can face criminal charges for engaging in acts not considered criminal if done by a person who is HIV negative.

On April 30, 2025, medical students, health care advocates and future physicians gathered for an energizing advocacy workshop led by Lindsay Cobb, senior associate at the United Nation World Immunization Shot@Life event at Drexel. What followed was more than just a presentation — it was a masterclass in mobilizing passion into policy.

Menstrual health is an essential aspect of women's health that often goes underappreciated. For immigrant and refugee women in particular, managing menstrual health presents unique challenges. Cultural differences, language barriers and limited resources all contribute to these challenges.

I came to medicine from the world of ballroom dancing. While I knew that my stethoscope would be joining me far more often than my dance shoes, what I did not expect was how many lessons from the ballroom world would shape my learning and working in the clinical space. So many of the cardinal rules of ballroom dancing, also known as partner dancing, apply to medicine.

Pregnant people in the United States have many options when it comes to planning what their labor and delivery experience looks like. Common options include home delivery, various types of delivery centers and the hospital. In the United States and other western countries, hospital deliveries have largely become the default. Each option comes with its own benefits and downsides.

Intrauterine devices (IUDs) are an increasingly popular choice for contraception. There are two types: hormonal (which contain progestin, a form of progesterone) and non-hormonal, made with copper. You can discuss with your health care provider which one is best for you.

We all have an organ called the pancreas. The pancreas produces a hormone called insulin. Insulin acts to regulate your blood sugar levels, making sure that they don’t get too high and that your cells get all the energy they need! However, there are many changes that happen with the body during pregnancy; sometimes your pancreas is not able to produce enough insulin to maintain a normal blood sugar. This continually high blood sugar is called gestational diabetes.

In today’s digital age, social media has become a central aspect of adolescent girls’ lives. Platforms like Instagram, TikTok and Snapchat are among the most popular, offering spaces to connect with friends, share content and explore interests. While social media offers many benefits, including connection, self-expression and entertainment, it can also negatively impact mental health.
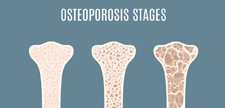
Osteoporosis is a common disease that results in bone weakening and increased fracture risk. Its prevalence is higher in women than men and has continued to increase in women from 2007–2008 to 2017–2018 according to the CDC.

Pregnant women are at risk of developing another type of depression called postpartum depression (PPD). The symptoms for postpartum depression and major depressive disorder are the same, with the exception that postpartum depression develops within a year of giving birth or within the last trimester of pregnancy.
Pregnancy is a unique period in a person’s life. During these 40 weeks, the body goes through many changes and adjustments to nurture the fetus growing inside. One common complaint, present in about 50-80% of pregnant patients, is low back and/or pelvic pain. As the patient gains weight, the center of gravity is shifted forward which increases the forces applied to the lower back. Back pain has also been correlated with increased levels of relaxin which is a hormone produced by the corpus luteum and uterine decidua.