On a Mission
How do you leave your practice for weeks on end, plunge into daunting conditions where crowds of patients await your skills, and give more care with fewer resources than would even be deemed possible at home? "It's a privilege," says alumna Libby Wilson. "It makes me grateful," says Sue Benes. "I was lucky," says Gerald Rothacker. This culture of service is a common thread from the legacy schools — Hahnemann, Woman's Medical College and Medical College of Pennsylvania — to Drexel University College of Medicine. But the "pioneers" report some harrowing learning experiences.

Sue Benes, MD, MCP '75
Sue Benes, MD, MCP '75, is a neuro-ophthalmologist who has traveled and served all around the world. She recently moved to Colorado after 35 years of practicing in Ohio and teaching residents at The Ohio State University College of Medicine.
My first opportunity to travel overseas was in 1980, when the government of Kenya asked the U.S. to provide a volunteer faculty for the first class of ophthalmology residents on the continent of Africa. We also set up a clinic out in the country.
We'd go village to village assessing how many people were ill, needed medical treatment, or needed surgery. The most prevalent need was for cataract surgery. We'd ask the leaders of the village to vote for a person who'd be their clinical officer or liaison between us and the village, their "barefoot doctor." We'd teach them how to screen height, weight and head circumference, how to have clean water and how to separate waste from the water — basic preventive medicine.
Since the new ophthalmology residents in Nairobi were too far away for these rural villagers who were blind from cataracts, we'd set up a day for the blind at nearby Nyeri Provincial General Hospital. We'd teach the clinical officer, slowly but surely, how to take out cataracts of their relatives and neighbors. It probably wasn't strictly legal, but it was the quickest way we could think of to get enough trained hands to help the Kenyan people.
The villagers accepted us because we were working as a team with somebody in their own village. Also, I took my 5-year-old daughter with me. I think it broke the ice to have a lady who was a mom and was also a doctor.
MAKING AMENDS
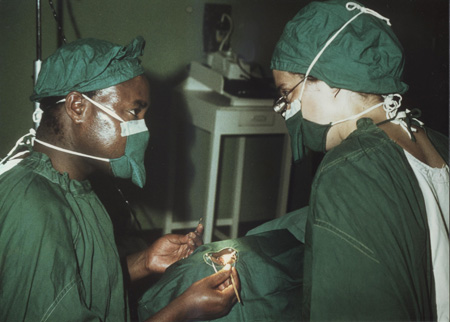
Dr. Benes (right) teaches a non-physician, "a village barefoot doctor," how to take out a cataract in Kenya in 1980. Note the bare hands and lack of light.
Later I was recruited by the FBI to work with the Department of Energy in the Marshall Islands, helping people who had been exposed to radiation from U.S. nuclear tests [which took place between 1946 and 1958]. The testing was done on islands that had been evacuated, but the fallout resulted in many people being irradiated. We were so ignorant, at the time, of the power of atomic energy that we even miscalculated where the winds would go.
We volunteers took an old barge and turned it into a hospital. Then we'd go from atoll to atoll, bring people to the ship, and check them. Thyroid cancer was really prevalent.
If I thought a person had thyroid cancer, they needed an ultrasound-guided biopsy. If the biopsy was positive, they'd need a thyroidectomy. The government gave us money to fly the person and their spouse — it was mostly women with thyroid cancer — to Hawaii for the ultrasound and biopsy. Then they'd be flown to the Cleveland Clinic for the thyroidectomy. Then to Washington, D.C., where they'd undergo another series of tests — kind of a whole-body Geiger counter. Then they'd fly home to the Marshall Islands, and there would be a cash settlement. The men would take the money. In that culture, the men own the money, and the women own the land. The woman would stay on her land, and the man would move on to another lady with a big neck.
We had good intentions to do the right thing by these people, but it never occurred to us that when you make a system, people quickly learn how to take advantage of it.
In the village of Utirik on Utirik Atoll, a 98-year-old woman told me this story: A Russian sailboat landed on their beach, and the Russian sailors told them, "You live in paradise on earth. The only thing Russia has that's better is this stuff you can go sliding on or skiing on. You can go down mountains. You can make little balls of it and roll the balls, and build a man." On the beach, the Russians made angels in the sand and said you could do the same thing in snow. People were trying to picture this. So when our bomb testing created white fallout, people thought God had sent them a miracle. They sent the children out "to play in the snow." These children died of gamma poisoning. One of the woman's sons died of leukemia. So here she is, 98, telling me this story. It became clear how we'd changed the lives of these people.
MAKING DO
Three years after the Soviet Union fell, I went to the Republic of Georgia. No longer was there any electricity, gas, water, or money from Moscow. The Russians took the medical supplies and surgical instruments and closed the hospitals. So the Georgian doctors couldn't take care of patients. The chairman of ophthalmology there wrote to America and said, "Please. Send us someone to bring us aid."
We landed in Tbilisi at 3 in the morning. Underneath the plane, I had 18 crates that we had to figure out how to unload without power for the electric conveyors and automatic doors. Each Georgian doctor was allowed to bring one patient — the sickest. So 175 doctors and 175 patients were standing in a row at 3:30 in the morning, outside of a closed-off hospital, trusting the Americans would come and bring the equipment and medicine.
We'd do surgery with the doctor who had brought the patient. They hadn't been able to do any surgery in four and a half years, so they were rusty. I brought a generator so we could generate enough electricity for a surgical microscope. We brought buckets so we could make a bucket brigade from the creek to flush a toilet.
RISK/REWARD
Every time I went overseas, I was making no money, but I still had practice expenses at home: rent, loans for my equipment, employees and their benefits. That risk was well worth it. It inspired me to come back re-energized. It made me more grateful for the blessings we have in this country. Having seen bad things our country may have inadvertently done, but how we stuck with the people and decided to make it right — that makes me prouder to be an American. I'm so grateful I have the freedom to do these things, to serve as an American to try to make the world healthier.
I'm also grateful to my ancestors who were physicians who served overseas and made me dream of doing service work when I was just a child. One of them was Dr. Jessica Royce Carleton, who graduated from Woman's Medical College in 1886 and lived the rest of her life in India serving in a hospital for women and children, teaching medicine and surgery. I will also be eternally grateful to those who taught me at WMC/ MCP/Drexel and at the Wills Eye Hospital (residency and fellowship), as they gave me the academic and practical knowledge to know what to do in many different places in the world, and to touch and care for people with respect and compassion wherever I am.
Back to Top

Gerald Rothacker, MD, HU '76
After several attempts at mission work that didn't quite "fit," Gerald Rothacker, MD, HU '76, found his connection with Mbingo Baptist Hospital in Cameroon and has gone there annually for the past five years. Recently retired from his orthopedic practice in Lancaster, Pa., he is already planning his next trip to Cameroon.
I always wanted to do mission work, to give back, but I never felt like I had the opportunity. I went to New Orleans after Katrina, but that was mainly construction. When the earthquake hit Haiti in 2010, another mission opportunity opened. That was truly my first overseas mission experience, yet I came back thinking, "That's neat, but that's not where I should be going."
The following year, I went on a mission trip in Iraq, to Erbil in the Kurdistan region. Our task there — we were actually hosted by the Kurdish military — was to help open a mothballed hospital facility. Every day we ran clinics for the Kurdish military, their families, and friends. That was a fascinating experience, but it didn't use my skills as an orthopedic surgeon.
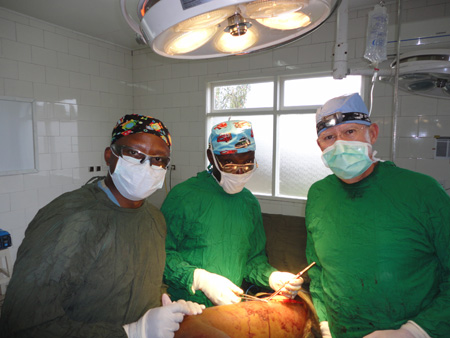
The equipment may be old and dull, but you use what's there, says Rothacker (at right). What stands out is the people.
Then the door opened for me. One of my partners went to Cameroon through Samaritan's Purse, an international relief organization. He met a general surgeon there from the United States who was a long-term missionary. That fellow, Dr. Jim Brown, came to Lancaster at my colleague's invitation and delivered a presentation on what he was doing at Mbingo Baptist Hospital in northwest Cameroon. He presented an unbelievable wealth of pathology and basically invited all the doctors there to come over. I thought, "This may be just right."
INTO THE BREACH
So in November of 2012, I went to Cameroon through Samaritan's Purse as well. It was an enlightening experience. About 80 percent of the patients I treated had fractures, and many had been neglected for months — or even years — until the patients were sure they weren't going to recover or until they could afford medical care. In Cameroon, patients do not go into surgery until they've paid the bill, even for open fractures that are through the skin — they get washed and put in a splint. There's an occasional exception if a person has absolutely no financial wherewithal, for example, a widow or an orphan; the hospital will give them the opportunity to pay after they've been treated.
I see kids with deformities, often because of vitamin D deficiency. I also treat a lot of children with chronic bone infections, not from injury, but from an infection like strep. That was not uncommon in the United States 60 years ago. But in my 35 years of practice, I had never seen a true chronic osteomyelitis — where a child had an ear infection or strep throat, and the bacteria in the bloodstream spread into a bone. In this country, if that happens, it gets treated so quickly, it never gets to the stage we call chronic.
Mbingo Baptist Hospital is about 250 beds [about the size of Pennsylvania's Easton or Chester County Hospital]. But it's a Cameroon hospital, and in Cameroon hospitals, the patient's family provides for the basic needs of the patient. The family takes care of the meals and hygiene. The nursing staff does vital signs, changes dressings, and passes out medicines.
The equipment we use is basically 1950s–1960s style and donated from the United States. Surgery is done by looking at a preoperative X-ray, judging where you have the pieces, and hoping they're all right when you finally do get another X-ray after the surgery. There is no X-ray available in the operating room. That's now completely foreign in the U.S. We're so dependent on our image intensifier X-rays.
When it comes to the things we implant, like plates and screws, you have to use what's there. Many plates are reused when they've been removed from a patient. The first year, I was sort of shocked. This last year, it didn't shock me anymore. It's just the way it is.
What stands out is the level of devotion people have. Dr. Brown belongs to PAACS, the Pan-African Academy of Christian Surgeons. It was founded by a doctor-missionary about 25 years ago. He realized that he'd helped thousands of people, but when he retired, they'd be left just like they were before. So he started PAACS to train African doctors as general surgeons to stay in Africa. The goal is to have trained 200 surgeons by 2020. I usually have one of the surgical residents assigned to me, so I get to teach some orthopedics for the two weeks.
Physicians reading this are going to say, "That's interesting. What that guy did, I would like to do. He was lucky to find this Dr. Jim Brown to open the door." I would just put in a plug for Samaritan's Purse. They're always in need of doctors. Anybody who's looking for that door and wants to pull it open and see opportunities — that would be the place to start.
Back to Top

Libby Wilson, MD, WMC '63
Libby Wilson, MD, WMC '63, a pediatric plastic and reconstructive surgeon in Los Angeles, is an expert in cleft palate and other craniofacial reconstruction. She has lent her skills to healing children and training colleagues in Cambodia, China, Israel, Peru, the Philippines and other countries throughout her career.
Cleft palate is not limited to one specific ethnic group. It affects everybody. You can minimize a very obvious birth defect that might have prevented someone from being able to achieve the goals in their life.
Other conditions are endemic to certain areas. In 1979, I traveled to Sri Lanka, where the population that works in the tea fields chews betel. (Betel chewing is common in many Asian cultures for its psychoactive properties.) The betel nut itself is not carcinogenic, but to get the alkaloid released, they soak it in lime. You put that in your cheek, and eventually a cancer tumor develops. Ultimately the inside of the cheek eats through. I was there to reconstruct the cheek after the tumor was removed.
I try to read up when I go anywhere I haven't been before — find out something about the culture, and if possible, talk with someone from that country who's here in the States.
My next trip was to Yucatán with the Friends of the Americas. We worked at the Social Security Hospital and reconstructed a number of adults with cleft palates and tried to train local surgeons to do the surgery. Training became one of my subsequent goals. The service is wonderful for the families, but training sustains the work. That was the dawning of, "If you're going to do something, you've got to visit multiple times and establish something that is self-sustaining."
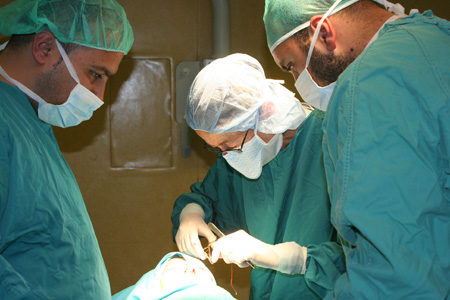
On a trip to Israel, Libby Wilson (center) worked with surgeons who perform cleft palate surgery on the West Bank.
BUILDING RELATIONSHIPS
My sister and I went to Nepal in 1984 to go hiking. I fell in love with the country. Everybody goes because they want to hike, and you just fall in love with the people.
The next year, I went back and worked with a clinic with a religious affiliation. They introduced me to the chief of surgery at the Teaching Hospital of Tribhuvan University Medical School, which was the only medical school at the time. A year later, I went back with a group from Interplast (a nonprofit that provides free reconstructive surgical treatment to those in urgent need around the world). On that trip we got the local surgeons involved and continued their training. So now we have two cleft palate programs in Kathmandu. They established that they repair the lip at 3 months, the palate at 10 months, and the gums at 10 years. They have that ongoing relationship with patients.
Our last working trip to Nepal, in 2001, was to one of the Zonal Hospitals. We had a person trained in Kathmandu who did the follow-up. Those trips are interesting because you have a hundred people show up on day one. Everybody in Nepal had a radio, and public address announcements were broadcast just before the news. They'd hear the message and start walking. In Nepal, it can take 10 days to get from your village to a paved road where you can catch a bus to our location. And that's an overnight bus ride. They'd all be there waiting when we arrived.
We'd get them organized into some kind of a safe schedule once we checked out the equipment and made sure we'd have an anesthesiologist. We had speech pathology and dentistry. We'd bring a whole team and work with our counterparts. We'd organize a day of lectures — a real professional meeting. It was probably my longest association and definitely personally rewarding.
More recently, I've been going to Peru, to a community on the plateau, Ayacucho, with a group from our hospital. I've been doing that for about five years now. We've seen the kids coming back, and it's nice to see that. I have plans to go back to Peru in June 2017.
TREAD SOFTLY
It's a real privilege to do what I've done in the areas where I've been. It's about what gets accomplished in the appropriate way. It's really important to understand what the local situation is. Go in with an open mind, not a preconceived notion. Remember what you're offering may or may not be a high priority where you're going. That's why it's important — though you may not get a full sense — to try to read something about it in advance. Then find someone who is an ex-pat from the area.
A story that is meaningful to me was told by an anthropologist who spent three years with a Mayan group outside of southern Mexico. He spent the first month just sitting on the corner of the plaza, not interacting with anybody. "I just wanted them to get used to seeing me," he said. You don't enter loudly. Walk in quietly. Observe. Don't jump into the middle and do before you have a chance to observe and see what's going on.
You want to build a legacy that's not dependent on your coming back all the time. Somebody is there to take over. That, to me, is a very important principle.
Back to Top