Education for a New Generation
By Elisa Ludwig
No doctor works in isolation, and students need to be prepared for the rapidly changing, increasingly collaborative health care environment of the 21st century.
A new curriculum — to be launched in August 2017 — recalibrates Drexel University College of Medicine's approach to medical education, emphasizing community, cultural competence, team learning and professionalism in preparing students for practice in the real world.

Medical students can come and go by shuttle bus between the Queen Lane Campus and Center City. The Queen Lane lobby is pictured here.
Two years in the making, Foundations and Frontiers will replace the current two-track system, merging the best aspects of both, together with exciting innovations, into one unified program. The new paradigm recognizes the imperative to equip students for a different reality, with both the qualities essential to clinical excellence and the emerging competencies required in today's world.
"We're fundamentally changing how we think about training the physicians of the future," says Valerie Weber, MD, MS, FACP, vice dean for educational affairs. "It's no longer simply about acquiring a body of facts through lectures and reading, and repeating that information back during exams, but about giving students skills to continually apply and update their knowledge."
A RENEWED APPROACH
Medicine has changed dramatically over the past few decades due to shifts in financing, organization and the delivery of services. Physicians are increasingly expected to deliver higher quality and more efficient care, and to work in teams. With a continually expanding foundation of "best practices," medical professionals are also expected to stay abreast of the latest information.
The existing College of Medicine curriculum focuses on two years of basic science followed by two years of clinical work, with students choosing one of two tracks. Foundations and Frontiers is a single-track, four-year program divided into three phases: Foundations, Applications and Transitions.
Foundations lays the groundwork with basic and clinical science during years one and two. Studies begin with cells and tissues and proceed into organ-based learning blocks with a focus on normal processes. The focus shifts to abnormal processes in year two. Students have early and frequent clinical exposure starting in their first year.
The Applications phase allows students to extend their patient care knowledge and skills to a variety of clinical settings during year three. Students will participate in a transition session to prepare for their clerkships and then pursue rotations in surgery, internal medicine, family medicine, pediatrics, psychiatry, obstetrics and gynecology, and neurology. To enhance the diversity of their clinical experience, students will work with faculty at multiple sites, ranging from metropolitan medical centers to neighborhood practices to rural clinics.
In the final Transitions phase, students focus on advanced clinical preparation for residency. With a Pathway adviser, either focusing on a single discipline or a broader set of experiences, students take both required and elective classes as a gateway to the next phase of their training. Students can also complete a number of elective rotations at non–Drexel-affiliated institutions, including international hospitals, health centers and clinics.
FRONTIERS
During four 1-week blocks in the Foundations phase, students begin their engagement in the Frontiers component, where they focus on cutting-edge topics in collaboration with Drexel's other colleges, fully taking advantage of the University's offerings. These include health informatics, population health, quality and patient safety, biotechnology, health care systems and financing, and principles of translational research.
In the Transitions phase, fourth-year students can choose advanced studies in one select Frontiers area, including population health, health care administration or health care informatics, with the opportunity to earn a concentration. Alternatively, they can conduct a scholarly project under the direction of a faculty member.
THE CALL FOR CHANGE
Created with input from students, faculty, alumni and medical education experts, Foundations and Frontiers builds on the College of Medicine's legacy of medical excellence and innovation while embracing the larger University's strengths in other areas. It also represents a cultural shift in medical pedagogy that has been observed over the past several years, from didacticism to a learning-by-doing approach.
The 2010 Carnegie Foundation for the Advancement of Teaching report Educating Physicians: A Call for Reform of Medical School and Residency examined the issues facing doctors today and offered a blueprint for educational transformation. While the traditional culture of medical education was autonomous, expert-centered and hierarchical, this emerging culture values collaboration, transparency, a service orientation and patient-centered care.
Among the report's recommendations were to immerse students in clinical experiences earlier; integrate basic, clinical and social sciences; create long-running connections with patients; emphasize teamwork; and allow for continuous improvements in the learning environment.

Students come to class ready to discuss what they have learned through online tutorials, videotaped lectures and reading assignments.
A FLIPPED CLASSROOM
These principles guided the College of Medicine's development of the new curriculum. Instead of treating medical education as a finite set of teachings, students will be given models of how the body works and the problem-solving skills to engage with the always-evolving science.
Learning Societies
Incoming College of Medicine students will have the best of both worlds — the academic foundation from a large, top-rated university, and the more intimate and supportive experience of a small school. Introduced in 2015, Learning Societies foster a sense of community for both students and faculty. The four cohorts were named by last year's first-year students in honor of Philadelphia monuments (The Athenaeum Society, The Liberty Bell Society, The Physick House Society and The Rocky Statue Society). Each first-year student is placed in one of the societies, joining second-year students, faculty directors and faculty mentors.
The Learning Society provides a framework for long-term relationships between students and faculty, encouraging study on a collaborative basis both in class and beyond. Each society is guided by faculty advisers and student representatives who are responsible for coordinating and planning activities, such as community service projects, wellness activities, career advisory events and learning competitions, in addition to social gatherings.
"We drew from the Flipped Classroom model, which initially came out of K–12 education," Dr. Weber says. "The idea is to give students the opportunity for knowledge acquisition ahead of time and use class time to apply that learning."
The new curriculum also integrates technology-based learning in a number of ways. The delivery of information caters to tech-savvy learners who tend to be more self-directed, with online video and tutorial components as well as independent assignments to be completed outside of the classroom. Through these technology-enhanced instructional formats, using Drexel-developed iPad applications, students can take in information at their own pace before coming to the classroom. They will then use class time to process, integrate and apply their knowledge.
Students will also take advantage of the College of Medicine's state-of-the-art Simulation Center. In the Applications phase, students will log their experiences into a smartphone or iPad and support their real-time learning with an online program, videoconferencing for discussion and virtual "web patient encounters."
In essence, students will spend fewer hours in traditional lectures, which reflects their growing preference — in recent years, most students have relied on streaming video rather than attending lectures in real time. Instead of nine classes in individual subjects the first year, they will take four, with classes merging disciplines such as genetics, biochemistry and cell biology for a more holistic approach. Courses across the Foundations phase include Molecules to Organs, Human Structure and Function I and II, Foundations of Disease, and Disease Systems I and II, designed to integrate study in the same way the body's systems are integrated.
Microanatomy course director Haviva Goldman, PhD, for instance, is teaming up with Gross Anatomy course director Dennis DePace, PhD, to develop learning activities for the new curriculum. "We're working to maintain the integrity of our subjects but trying to be creative in our delivery and help students integrate their knowledge so that they come away with what they need to be medical practitioners," Dr. Goldman says.
In anatomy, students will still get the fundamental experience of working with cadavers, but the emphasis will move away from memorization. "We believe thoroughly that the act of dissection is what the students need to understand the threedimensional nature of the anatomy," Goldman says, "but we want to help them focus in on the key points that they'll really need to remember as they move through their careers."

Students will have early and frequent clinical exposure starting in their first year.
Classwork will emphasize problem solving, as students will be continually prompted to apply their knowledge to clinical cases. Learning will be more collaborative, with teamwork in classes and in small groups formed in a student's Learning Society [see sidebar, page 11]. The goal is to produce doctors who can think critically in a clinical situation and work successfully with interprofessional teams. In a hyper-connected, data-rich environment, doctors may no longer be expected to know everything about everything, but they must know how to find the answers they don't have.
"The reality is that in modern health care, even if you have your own private practice, you are still working with nurses, physician assistants and office staff, and you need to be able to work with that group of people to achieve a common goal," says Michael White, PhD, course director for the Physiology and Nutrition courses. "Everyone on the team has something to say, and the collective knowledge of the team is greater than one person can provide."
A critical component of the new curriculum is case-based learning, in which small groups of students meet with faculty facilitators to analyze a clinical case. The cases integrate social, behavioral and ethical principles, as well as the basic science being covered that week. The objective is to help increase their clinical reasoning skills and bring basic science to life.
For example, in Human Structure and Function II, one of the cases might be a patient with congestive heart failure. "Students will need to understand what drives the heart rhythm, how the contraction of the heart is controlled, how blood pressure works and what compensatory processes come into play," Dr. White says. "The session won't explain everything to students but will prompt them to investigate what they need to know. Students will be expected to take charge of their education, which in turn will help them become agile thinkers with the ability to constantly integrate new knowledge."

A student reviews information in preparation for discussing the case of the week.
PROFESSIONAL AND PERSONAL GROWTH
Community engagement is another cornerstone of the program. Expanding on the College's longstanding commitment to both community service and patient-centered care, students will participate in the Longitudinal Community Care Practicum, an interprofessional, community-based learning course that offers exposure in multiple dimensions over the course of the first two years of study [see Longitudinal Community Care Practicum].
Longitudinal Community Care Practicum
Too often, medical students don't have the chance to develop long-term relationships with patients, but an important component of the new curriculum gives them that opportunity. For the first 18 months of their studies, students will participate in the Longitudinal Community Care Practicum. Working alongside nurses and other health professionals, students will get to know patients and follow their care over time, whether it's a pregnancy or treatment for an illness.
Designed to offer a better understanding of the patient experience, the practicum also explores the real-life challenges of the health system. Students will not only gain experiential learning through patient partnerships in nonclinical settings, but they'll also investigate social determinants of health and the consequences of health disparities, and develop on-the-job professional experience through reflection and group inquiry, all of which contribute to professional formation and the curriculum's emphasis on patient-centered care.
As ever, professional formation remains a critical thread in the program. Students will be continually encouraged to develop their empathy and compassion for patients, cultivating skills of mindfulness, self-reflection and self-regulation.
Students will reflect on the impact their medical training has on them personally through discussion and writing. "They will have a chance to process their experiences, such as seeing their cadaver for the first time or experiencing the death of a patient," Vice Dean Weber says. "There are many facets of this experience that can be challenging on a personal level, and we want to provide the support to help them become excellent clinicians."
Given diverse patient populations and disparities in health care, today's physicians must be culturally competent. Foundations and Frontiers emphasizes the development of these crucial skills from the outset of student learning, with specific threads that help them better understand patients and colleagues from different backgrounds, improve communication and bridge the gap across cultures, biases and belief systems for more effective care.
Last year, as the nation's cohort of new doctors graduated, one in 75 set forth with an MD degree from Drexel. Weber believes the College has a responsibility to ensure the next generation of physicians are competent, compassionate and active learners. "Embracing a new curriculum is not easy, but we have had outstanding input from alumni and faculty. No one has shied away from this process and what it demands. In the end, we all want to improve the health care system, and this transformation will help us continue to turn out top-caliber doctors who can face the new challenges ahead."
Simulation Center Orientation Game
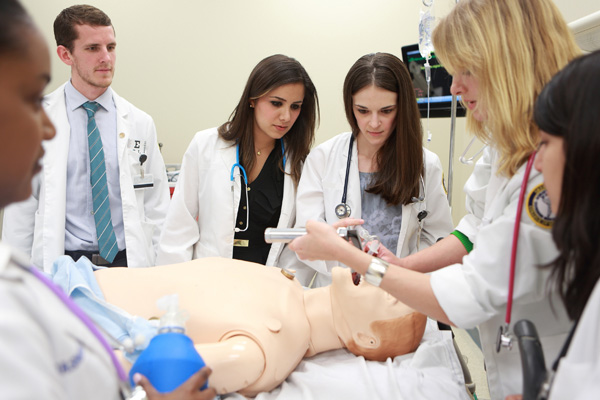
Drexel's incoming medical students will have the opportunity to prepare for the academic — and technological — challenges ahead with a leadingedge orientation game, developed by Web application developer Greg McGee and Drexel's Technology in Medical Education co-op students. The 3D game offers an entrée to the Simulation Center, where students learn from high-fidelity mannequins.
When students log on from their computer, they encounter the Sim Center's training room, where they learn its basic commands and controls, and meet their virtual team members. From there, they move into a 3D model of the Sim Center with four different clinical scenarios to test out. In each, they are faced with a patient in a critical situation; the objective is to stabilize the patient while working with team members to provide fast and efficient care.
Current students are now testing the program's beta version, and the game will be available for use during the 2016–2017 academic year.
Editor's Note: Special thanks to Donna Russo, PhD, HU ‘89, senior associate dean for curriculum and professor of microbiology and immunology, who provided extensive background information for this article.
Back to Top