Talking to Kids about Weight: What the Internet Says and Why Researchers Are Wary

Parents, caregivers and health care professionals are increasingly concerned about childhood obesity. Compounding their concern are fears of inadvertently provoking disordered eating, such as unhelpful dieting, when discussing a child’s weight status (i.e. normal weight, overweight or obese). Given the complexity of these concerns, major health advocacy groups have independently published guidelines for having conversations with children about weight status – all at the fingertips of parents, caregivers and health care professionals with a quick internet search.
To help sort it all out, researchers from the Center for Weight, Eating and Lifestyle Science (WELL Center) in the College of Arts and Sciences at Drexel University systematically reviewed numerous independently published guidelines for having conversations with children about weight status to analyze their content, consistency, actionability and scientific support.
“It’s important that parents and health care professionals be critical consumers of guidelines on talking to kids about overweight and obesity because guidelines have a lot of variability between them on the question of whether or not to talk about a kid’s weight directly,” said Elizabeth Lampe, graduate student in the College of Arts and Sciences and lead author. “Parents and health care professionals should read several different guidelines and make sure that they are making the best decision for their kid, since every situation can be unique.”
Researchers performed web-based searches that identified 59 independently published guidelines on childhood obesity by major health advocacy groups. Only 13 provided explicit direction on how the caregiver or health care professional should approach a conversation about overweight or obesity with a child.
Throughout the 13 guidelines, nine topics were identified within the advice provided: attitude modeling (covered by 31% of guidelines), behavior modeling (61%), dietary recommendations (54%), physical activity (46%), body acceptance and self-esteem (69%), conversation advice (92%), contact with health care professionals (46%), talking about “weight” versus “overall health” (54%) and external factors, such as bullying and/or media (54%).
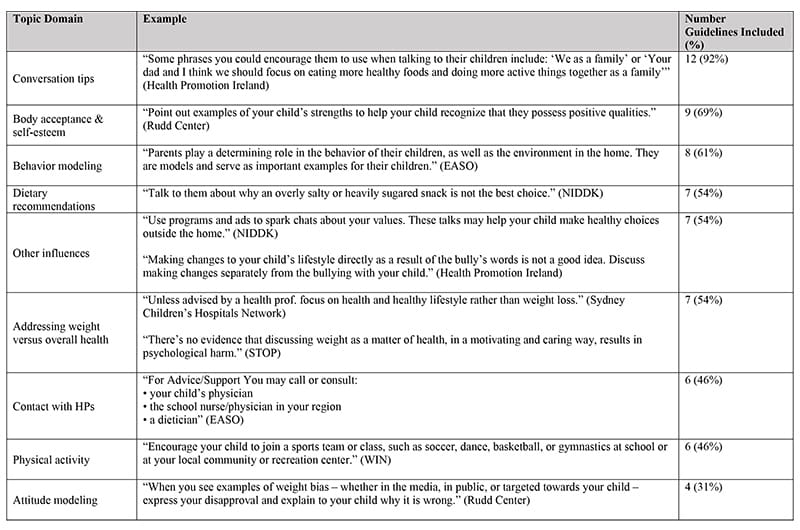
Lampe noted that although all guidelines presented similar content, several inconsistencies in recommendations emerged. Only three of the 13 guidelines referenced any scholarly sources and only a small minority of advice was easily applied to everyday situations by caregivers or health care professionals.
“We call for future guidelines to unify their messages for caregivers and health care professionals and be better supported by scholarly data,” said Lampe.
She added that parents and caregivers are not the only consumers of these guidelines.
“Policy makers may be using these guidelines to influence their decisions or practitioners might use these guidelines to inform their practice,” said Lampe. “Some important implications of this could be a lack of health behavior change and potential perpetuation of weight stigma.”
The report, “Guidelines for Caregivers and Healthcare Professionals on Speaking to Children About Overweight and Obesity: A Systematic Review of the Gray Literature,” was recently published in Translational Behavioral Medicine. Authors include Sophie Abber, graduate student; Evan Forman, PhD and Stephanie Manasse, PhD of Drexel University.
Although this study has concluded, the WELL Center continues to recruit for other weight management studies, including a teen healthy lifestyle study through the Child and Adolescent Program called Project REACH.