Can Community Members Deliver Naloxone to Reverse Opioid Overdoses — And Do It Faster Than EMS?
Equipped with naloxone and a smartphone app, community members can save lives in the fight against America’s opioid crisis, according to a paper from researchers at Drexel University’s Dornsife School of Public Health and colleagues published this week in The Lancet journal EClinicalMedicine.
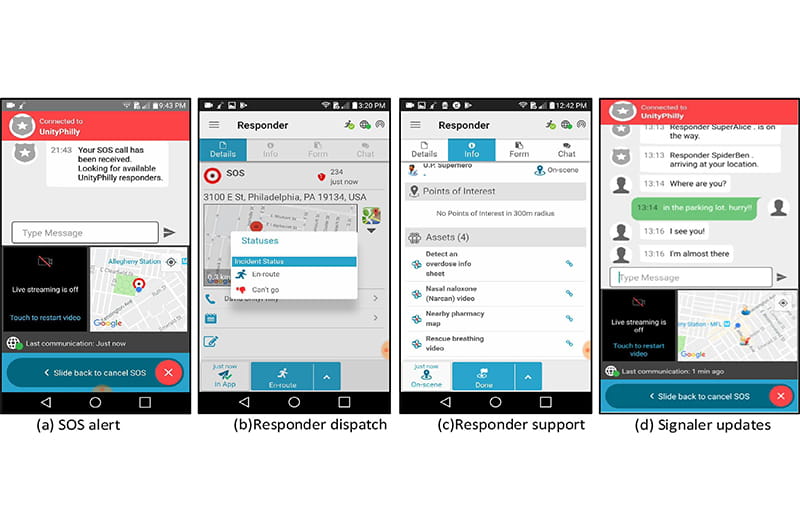
During a pilot study, researchers found that enrolled participants were able to signal and respond to opioid overdoses using a smartphone app, called UnityPhilly, developed by the study team. During 22 overdose emergencies, a participant received an overdose alert on the UnityPhilly app, traveled to the location and then administered naloxone to the overdose victim at the scene. In an additional 52 overdose emergencies, the participant who witnessed the overdose signaled an alert with the app and then administered naloxone themselves. A successful reversal was reported in 95.9% (71/74) of cases. In over half of these events (59.5%), study participants administered naloxone more than five minutes faster than Emergency Medical Services (EMS) were able to arrive on scene.
During the year-long observational study, that concluded in February 2020, 112 adult Philadelphians, 57 of whom use opioids, reported 291 suspected overdoses and alerted nearby volunteers using the UnityPhilly app.
All study participants were trained in how to administer naloxone, use the app and give rescue breathing, and then they were provided with two doses of naloxone. Every time an alert was signaled by pressing an “SOS” button in the app, it also alerted EMS via 911 which allowed them to follow up with their protocol, regardless of whether a layperson responded.
“We know that the lay public is effective at administering naloxone, but now we know that an app can help laypersons provide naloxone faster when every second counts,” said senior author Stephen Lankenau, PhD, a professor and associate dean for research at the Dornsife School of Public Health who co-led the study with David Schwartz of Bar-Ilan University, Israel. “By empowering community members with these tools, we strengthen the ‘chain of survival,’ and keep people alive until EMS or other medical personal administer further aid.”
Unless it’s reversed in time, an overdose from opioids, such as heroin, or pain relievers, like oxycodone or fentanyl, can cause breathing to slow or stop. Naloxone works as an antagonist that connects to opioid receptors to prevent the effects of other opioids in the body. Signs of an overdose include skin feeling cold, blue nails and lips, slow heartbeat and vomiting, among other symptoms.
In 2018, U.S. overdose deaths decreased for the first time in 25 years with 67,367 drug deaths, roughly seven out of 10 involving opioids, but that rate rose nearly 5% to an estimated 72,000 in 2019, according to the Centers for Disease Control and Prevention. The coronavirus pandemic is also suspected of raising overdose deaths and other “deaths of despair.” As of July 15, drug deaths are up 13% this year compared to last year, according to government data compiled by The New York Times.
Philadelphia has the highest per capita overdose mortality rate among large U.S. cities, with 1,150 deaths in 2019, a number up 3 percent from 2018.
The study focused on four Philadelphia zip codes, with participants recruited in the Kensington neighborhood, which experiences higher drug use and availability of naloxone than other areas of the city. The authors will next look at a city-wide study to test if the app can be scaled for all of Philadelphia.
Funding for this study was provided by the National Institute on Drug Abuse (NIDA).
In addition to Lankenau, authors contributing to this paper include lead author David G. Schwartz, of Bar-Ilan University, Israel; Janna Ataiants and Alexis Roth of the Dornsife School of Public Health; Gabriela Marcu of the University of Michigan; Inbal Yahav, of Tel-Aviv University, Tel-Aviv, Israel; Benjamin Cocchiaro, of the University of Pennsylvania; and Michael Khalemsky, of Bar-Ilan University.