Health in the City: Dornsife School of Public Health Research at APHA Annual Meeting

- U.S. Department of Education Provides Final Approval of Drexel and Salus Merger
- Spotting Bad Batteries Before They Malfunction
- When Climate Disasters Hit, They Often Leave Long-term Health Care Access Shortages, Drexel Study Finds
- New Research Highlights Health Benefits of Using Heritage Art Practices in Art Therapy

Earlier this week in Chicago, faculty from Drexel’s Dornsife School of Public Health presented their research on public health issues during the 143rd American Public Health Association (APHA) meeting and expo.
Drexel researchers’ topics covered a variety of areas, including air pollution, the effects of the Affordable Care Act in marginalized communities and what data breaches mean for monitoring disease.
Check out three highlights from the Dornsife School of Public Health's slate of presentations.
High Levels of Air Pollutants Correlated to Chronic Health Condition Rates
A significant association between elevated air pollution and the occurrence of several chronic health conditions was uncovered by a team of public health epidemiologists, environmental health and environmental engineering experts from Drexel.
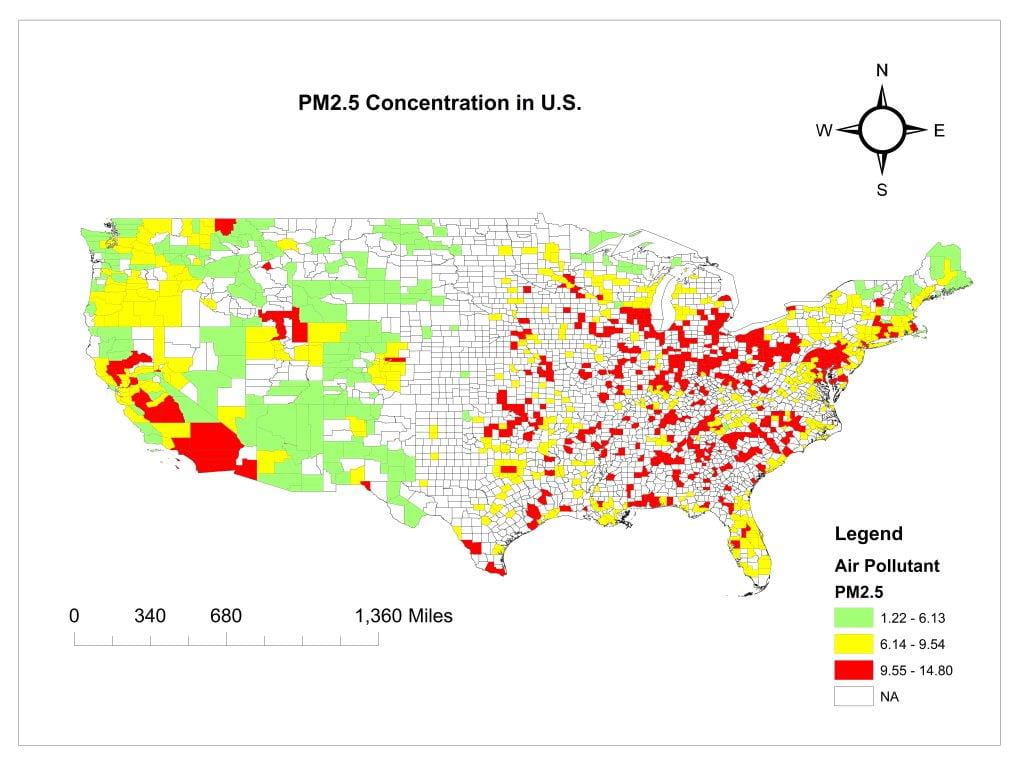
Heart disease, stroke, diabetes and hypertension, along with all-cause mortality, were found in a greater percentage of people living in cities and counties with higher air pollution indicators, found a Drexel team led by Longjian Liu, MD, PhD, associate professor of Epidemiology and Biostatistics. Early results from this analysis — comparing Environmental Protection Agency (EPA) daily air surveillance data with Centers for Disease Control and Prevention (CDC) health outcomes data — found the greatest correlations in the northeastern and southeastern parts of the United States.
Liu and his team are continuing to analyze data — looking at pollution levels during different times of year, levels between cities and levels compared to other countries — to measure the impact of climate change on the health of urban and suburban populations.
Neighborhood Income Levels Associated With Type of Health Care Providers Regularly Used
Studying neighborhoods in Philadelphia and its surrounding suburbs, a team of Drexel researchers found that the socioeconomic status of a neighborhood is related to the type of provider residents rely on as their usual source of care.

The Drexel team led by postdoctoral fellow Mustafa Hussein, PhD, found that while residents of low-income neighborhoods were less likely to rely on physician offices for their regular healthcare, they were more likely to rely on community health centers and outpatient clinics.
Dornsife School of Public Health Dean Ana Diez Roux, MD, PhD, and Professor Robert I. Field, JD, PhD, both participated in the research that also determined that “safety-net providers” like community health centers help narrow the gap in health care access by providing services in these neighborhoods.
In light of increased demand for primary care services spurred by the Affordable Care Act, it is critical that community health centers have the capacity and resources they need to continue to provide care in these communities.
The Drexel team proposed several policies to support these safety net providers, the most important of which is that Congress should ensure adequate federal funding for the community health centers (40 percent of their revenues come from federal funding).
Insufficient Investments in Public Health Infrastructure and Legal Concerns Diminish Potential of National Disease Surveillance Program
Technical issues and limited public health resources are restricting a federal effort to spot outbreaks at the earliest possible point.
A team of experts from the Dornsife School of Public Health and Drexel’s Kline School of Law reported that technical woes and insufficient investments in public health infrastructure constrain the potential of an electronic infrastructure, known as BioSense. Biosense is sponsored by the Centers for Disease Control and Prevention and can automatically capture clinical data and monitor trends in clusters of symptoms.
In-depth interviews with state and local health officials, hospital personnel and legal officials from six jurisdictions in the United States found that fear of data breaches — and whether states that report data would be held liable for them — were a primary concern preventing wider participation in the federal program.
However, some states and cities have participated in the program to take advantage of its data collection and analysis capabilities to supplement limited epidemiological resources.
This study was honored Monday as the APHA Law Section’s Abstract of the Year for 2015. The research team included the Dornsife School of Public Health’s Jonathan Purtle, DrPH, assistant professor of Health Management and Policy; Esther Chernak, MD, Tom Hipper, and Jillian Nash Arot, all from the school’s Center for Public Health Readiness and Communication; and Robert I. Field, JD, PhD, professor of Health Management and Policy in the Dornsife School of Public Health and professor at the Kline School of Law at Drexel University.
A comprehensive list of Drexel University presentations and activities at APHA can be found on the APHA Annual Meeting website.
In This Article
Contact
Drexel News is produced by
University Marketing and Communications.