Training Mannequin Named in Honor of Surgery Professor
 By Frank Otto
By Frank Otto

- New AI-Technology Estimates Brain Age Using Low-Cost EEG Device
- How Does it Work?: Drexel Guardian App
- Five Ways Drexel Students Can Get Involved with the Community, as Seen at Civic X EarthFest
- Bolstered by Research Consortium with Drexel, Jefferson’s Sidney Kimmel Cancer Center Earns NCI Comprehensive Cancer Center Designation
Quickly scanning a campus map of Drexel will turn up a host of buildings named for prominent faculty or donors.
There’s the Papadakis Integrated Sciences Building, the Daskalakis Athletic Center, and W.W. Hagerty Library, to name a few.
But there's something a bit uncommon named in memory of an outstanding former faculty member at the College of Medicine: a sliceable, bleeding, training mannequin.
Morton H. Perlman, MD, served as a professor in the Department of Surgery for more than 30 years at Hahnemann University Hospital before retiring in 1997 and moving with his wife, Esther, to Ocean City, N.J.
After Perlman died in the latter half of 2013, his family wanted to memorialize him in some way at the University.
“We looked at what was in need from an educational standpoint,” said D. Scott Lind, MD, the Department of Surgery’s chairman. “Our residents, more and more, need to learn outside of the operating room. We looked at what sort of thing we could make a fund for and we came up with TraumaMan.”
TraumaMan is one of the products sold by Simulab Co., a Seattle-based business that produces medical training and simulation devices.
The TraumaMan mannequin is used to train medical students how to deal with complex cases in a safe setting. However, just because it’s a mannequin, it doesn’t mean the training is a simple routine.
“When you open an abdomen for someone who was stabbed or shot, there’s a special program for that,” Lind said. “It’s pressurized and colored dye comes out. There’s many components to TraumaMan.”
Covered in a material that mimics human tissue with anatomically correct markings, TraumaMan allows for students to train for multiple scenarios and surgical situations.
Lind said having a physical mannequin on-hand is invaluable for learning surgery.
“When you look at the simulations, we’ve got virtual reality and game simulators for laparoscopic angioplasty and other things, but there’s really not a good way to train for trauma,” Lind said.
Using a mannequin like TraumaMan gives the necessary hands-on experience a gaming simulation wouldn’t, which made it the perfect learning tool to put the Perlman memorial fund toward.
Running between $10,000 and $15,000, the training mannequin was much more affordable than a robotic simulator the College of Medicine has had its eye on.
TraumaMan won’t just benefit the college’s aspiring doctors but would also fill a need for cross-training.
“I think we’re going to enhance the TraumaMan training,” Lind said. “Not only residents can use it, but anesthesiologists and nursing students. We’re trying to do some interpersonal training.”
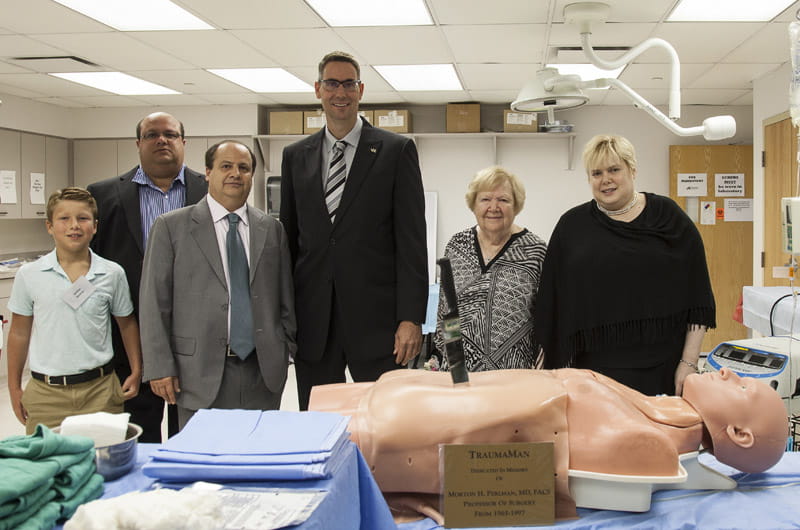
After the TraumaMan was purchased a few months ago, Perlman’s family came to meet the mannequin and posed for pictures with it. In a few of them, a large knife stuck directly in its stomach area.
Lind said the TraumaMan unit carries a plaque with Perlman’s name.
Having taught young surgeons for more than three decades, the addition of TraumaMan ensures that Perlman’s name will remain tied to the success of young doctors for many years to come.
Drexel News is produced by
University Marketing and Communications.