More than 37 million individuals around the world are infected with HIV. Within the HIV-infected population, there is a disproportionately large number of individuals who suffer from a variety of mental illnesses, the most prominent of which are substance use disorders. While drug abuse has long been associated with increased risk of acquiring HIV, research now shows that drug use also alters both the neuropathogenesis of HIV infection and the development of HIV-associated neurological disorders (HAND).
In this seminar at the Department of Microbiology & Immunology at Drexel University College of Medicine, Dr. Peter Gaskill discusses his laboratory's data on the impact of dopamine on HIV infection. His data show that dopamine increases the amount of HIV replication in primary human macrophages by increasing the ability of HIV to enter macrophages. His work indicates that this effect is mediated by activation of dopamine receptors present on the macrophage surface, and that both types of dopamine receptors, D1-like and D2-like, can mediate the increased infection. These data suggest that in macrophages, activation of both types of dopamine receptors triggers an increase in calcium flux through a non-canonical signaling pathway, and that this increase in calcium induces the greater amount of HIV infection. Overall, these data suggest that the changes in dopamine levels induced by drug abuse or the use of dopaminergic therapeutics could exacerbate the effects of HIV infection in the central nervous system. Further, these data indicate that neurotransmitters like dopamine are important players in neuroimmunity, and more focus should be placed on research investigating the role of neurotransmitters in the regulation of the neuroimmune response.
Several research projects in the Gaskill Lab focus on these alterations in the development of HIV neuropathogenesis, examining changes in the HIV infection process in macrophages, which are central components of the neuroimmune system. In the CNS, these cells are the primary targets for HIV, and their response to HIV infection is a central component in the development of HIV-associated neuropathogenesis. All drugs of abuse mediate their addictive and reinforcing effects by increasing CNS dopamine, so these projects examine the dopamine-mediated changes in HIV infection in macrophages. Our data show that elevated dopamine increases the susceptibility of macrophages to HIV infection, at least in part through activation of the endogenous macrophage dopaminergic system. These and other effects suggest that modulation of CNS dopamine may be a common mechanism by which different types of drugs of abuse can intensify the development of HAND.
Importantly, many legal therapeutics, including Abilify, Levodopa and Ritalin, also modulate the dopaminergic system, and a much larger group of neuropsychiatric medications, such as Prozac and Zoloft, manipulate a number of other neurotransmitter systems. While many of these drugs are widely prescribed, little research has been performed examining their effects on the neuroimmune system. The remainder of our research focuses on this question, examining the different mechanisms by which changes in monoaminergic neurotransmitters, such as dopamine and serotonin, alter macrophage immune function. Developing our understanding of the impact of neurotransmitters on macrophages in the context of CNS infection may enable us to devise new therapeutic strategies to directly counteract different types of neurological insults and boost CNS immune function.
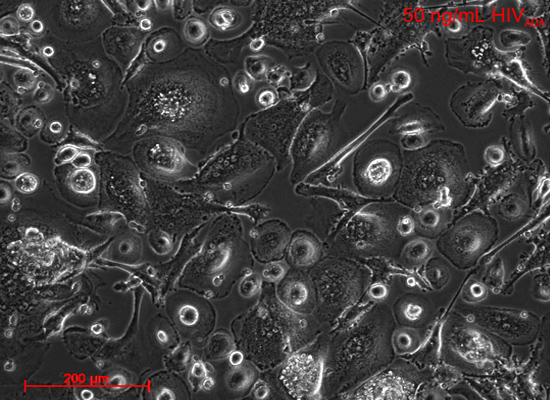
Brightfield image of primary human macrophages infected with 50 ng/mL HIVADA 7 days post infection.
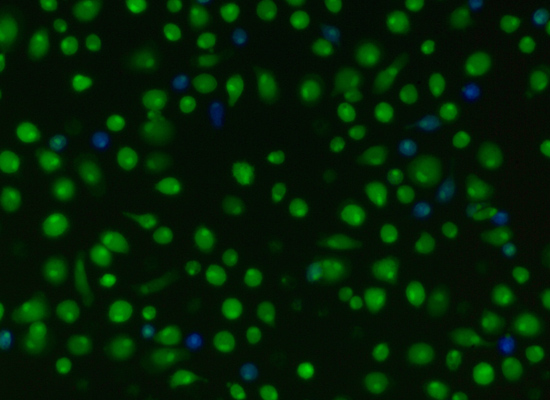
Measuring viral entry into primary human macrophages infected with HIVBaL in the presence of 10-6 M dopamine using a β-lactamase–based entry assay.

Imaging primary human macrophages phagocytosing 2 µm fluorescent microspheres using laser scanning cytometry.
*Banner image: fluorescent image of primary human macrophages infected with HIVADA in the presence of 2 x 10-5 M dopamine stained for nuclei (blue), actin (Texas red) and the HIV capsid protein p24 (green).
Back to Top